“You feel guilty. You want to quit but you can't” - Diary of a New York COVID Nurse

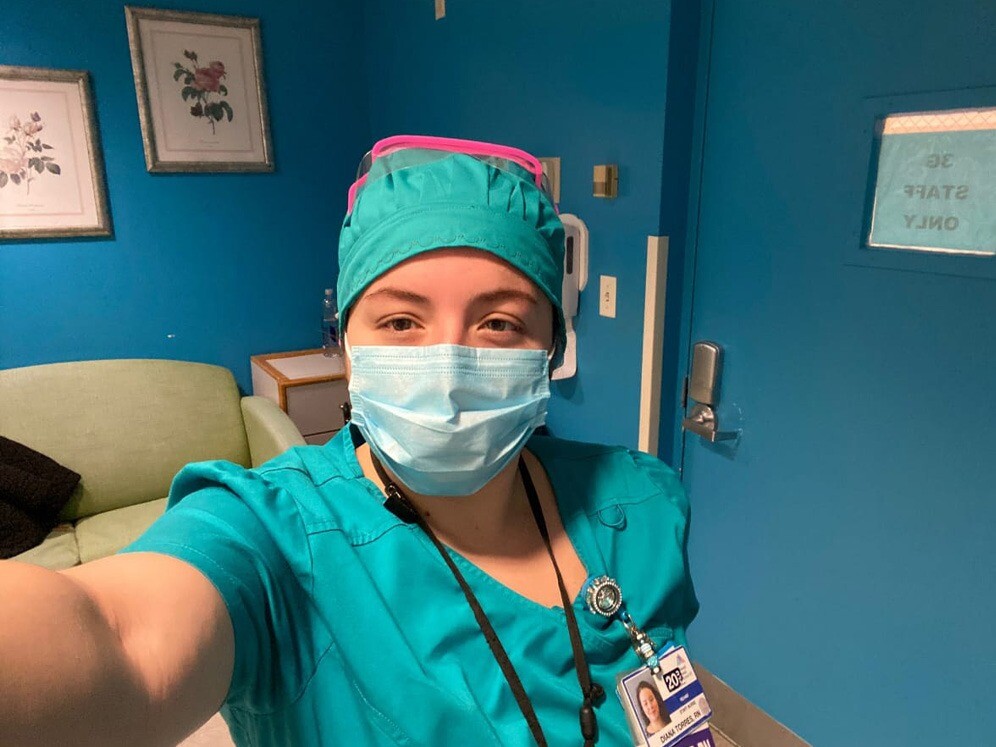
Diana Torres is a nurse at Mount Sinai West Hospital next to Central Park in Manhattan. In a journal of her experiences, she's sharing with RTD what it's like to fight COVID-19 as a healthcare worker in one of the pandemic's epicentres, New York City.
In an introductory interview, she talks about her experience as a nurse in the pre-COVID era, about the chaos the healthcare system plunged into due to the pandemic, about supply shortages, and working extra hours under the constant threat of being infected.
Diana Torres has been at Mount Sinai West Hospital for five years. Before the epidemic, she was assigned to the acute rehab unit: "it's very controlled, there's prior authorisation from the insurance, the patients have to be pretty stable medically so that they can manage three hours of therapy a day", she explains.
-7-br.jpg)
However, a restructuring of New York City hospitals has made her work far less predictable. The Wall Street Journal says 20 hospitals have been closed in New York City over the last 20 years – which brought the staff who had lost their jobs to her hospital, "so we ended up being overstaffed supposedly, and we started to float a lot in the past two years". Floating involves sending nurses to other units to cover staffing shortages. According to the nursing journal Nursing 2020, "for nurses, being sent to work on another unit where patient needs are different than those usually encountered in their home unit can evoke stress, anxiety, and frustration. Working with an unfamiliar patient population can ultimately threaten patient safety."
Diana worked in the orthopaedic unit, in oncology and medical-surgical units. "Some days if it's not too bad you may have four-five patients. On a med-surge floor when really bad it would go up to seven or eight between assigned, discharges and admissions", she says of her workload before the coronavirus outbreak. "It depends on the staffing and that changes by the second. [...] It just depends on how many people they have in the hospital on a particular day", she adds. Staff-patient ratios are a sore point for nurses. The State of California requires a ration of one nurse to five patients in medical surgical units.
"Our problems didn't start just because of COVID", Diana Torres maintains. "Our staffing issues had been around for a time", according to the nurse. In fact, "last year at this time we were supposed to strike. I think it was 11,000 nurses around New York City had given notice to start a strike a year ago on April 15", she recalls. They were fighting for staffing "so we could establish ratios and limit the amount of patients we can get because we were already struggling with not having enough nurses and having to pull from one unit to cover another".
Supplies, the Achilles heel of healthcare systems fighting COVID, were already a problem, the nurse points out: "We've had issues in my facility for about a year with supplies. Not having enough supplies, not having the proper supplies, having to borrow and get from other units, on a daily basis. Especially on the weekends, it was pretty bad."
-8-br.jpg)
Now though, things are on a different level. The first case of COVID-19 at the hospital was confirmed around March 10, Diana recalls: "We got the first patient, and it was complete chaos". Since then, "you show up to work, and you never know what you're going to walk into. It's never been completely predictable, but now it's so much worse". She says the hospital administration "isn't communicating very effectively" with staff.
One problem was that as patient numbers surged, Mount Sinai West quickly ran out of negative pressure rooms, which filter out the air. Hence, viruses breathed out by infected patients get sucked out, instead of stagnating and potentially infecting staff. For Diana Torres, "It was a disaster from the beginning, there was never actually a good plan".
COVID positive patients weren't put in rooms with others, but they were spread around the hospital: "They had to put the patients in regular rooms. Everything that's in there stays there. The virus is airborne; it's going to sit there for God knows however many hours or days".
They shared nurses with other patients "just from having the same nurse and being in and out of those rooms, even though you try to minimise exposure to yourself and the other patients", cross-contamination is bound to happen. The lack of proper personal protective equipment (PPE) in sufficient quantities has led to staff contaminating negative patients: "other patients that didn't potentially have the virus ended up with the virus after a couple of days or weeks."
For patients, the prognosis is grim and unpredictable. "The virus has played out to be pretty acute and dangerous for a lot of people, so you just can never tell how a patient is going to deal with the virus". Although many are discharged from hospital, others have to be intubated so that ventilators can help them breathe, "but they don't get extubated and manage to go home", she mourns. "A lot of people are dying. There were also people who were pretty young and healthy and didn't make it, so you just never know", she warns.
Her shifts, officially 12 and a half hours, often last 13 to 15 hours. "It depends on what kind of assignment you had and how your patient turns out throughout the shift". This was something that already used to happen, and is to some extent inherent to the nursing profession.
However, nurses aren't recuperating during their time off. "You can't rest." Mixed feelings of anger and helplessness stop nurses from switching off. "You feel guilty. You want to quit but you can't because you feel you could be doing more and you're not, or you're going to leave your coworkers, stranded and suffering on their own, while you're trying to save yourself", Diana Torres confesses. "When we're not working, we're still thinking about all of this and how this has affected our daily lives", she admits.
-9-br.jpg)
Protective equipment is a considerable worry for nurses. They wear disposable gowns, N95 masks, and gloves. "Sometimes you get given something to cover your head; sometimes you don't. Sometimes you get stuff to cover your shoes; sometimes you don't. They keep saying you don't need to cover your shoes". They also recycle masks.
"Whatever we're using hasn't played out to be very safe considering we're all pretty much infected and every day more and more people end up being sick", both coworkers and patients, concludes Diana Torres. "Nobody has been able to establish what is considered the proper PPE. It continues to be an argument and a fight. We keep telling them this is not enough, this is not OK, and nobody's hearing us", she denounces.
Testing is another sore point for medical professionals. Diana hasn't been tested. "I got an email saying that, because I'd had exposure from the beginning and I'd never had symptoms, I can go and get the antibody test to see if I can donate plasma". She's still waiting for a phone call telling her how and where to do this. "That could take another month or so; I don't know". Most of her colleagues who have been tested weren't tested inside the hospital "so that's not part of their strategy", she guesses.
The rules for sick leave are also unclear. According to Diana Torres, "every day, they consider different symptoms. At the beginning they said you had to have a fever, then they said it depends how high the fever is. At the beginning, if you had a cough or a sore throat or you weren't feeling well, you could stay home 14 days and that quickly changed to 7 days, and now it's 72 hours." She says that "some people had to come back to work coughing and not feeling well, so you just don't know. Nothing's established, there's no protocol, nothing in writing."
To alleviate staff shortages, the hospital has hired travellers, that is nurses coming from outside the area as temps, and also staff from doctors' offices and other facilities that are closed for the lockdown. However, "they didn't get properly trained so they're limited as to what they can do", regrets Diana.
Diana's hospital is private but takes in all patients. Because it's in a "good area", most patients have health insurance. Her colleagues working in the Bronx or Brooklyn report the population there is "completely different."
Nevertheless, the COVID epidemic has brought everyone to their knees. For Diana Torres, "this COVID thing has changed everything completely because there's no public or private, no longer poor or rich because everyone is getting it. It doesn't matter where you are. There's no longer VIP and specialty. We're just trying to survive and do the best with what we have because we're limited. We're all struggling for staff, supplies. It's the first time it looks pretty bad everywhere."
-10-br.jpg)
Diana Torres, a COVID Nurse Diary
15 April
So today I'm off, but I went to the protest. It was at one of the hospitals, Kingsbrook. We're all fighting for the same thing, making the same argument. We're all going through the same issues.

They're getting sick, they're not getting tested, they don't have enough PPE, and if they get it, some people get more than others; it's not established what's proper. We want full suits; we want to be covered completely. They're saying 'you don't need that, it's fine, whatever you're getting you should be OK, good luck to you!'
I picked up some donations and I took it to the hospital, and then later I dropped off at another hospital. We share the wealth. If we get any donations, I share with those who need it most. It's the same struggle throughout. This is not just in my facility; it's the same everywhere!
16 April
My first death!
-11-br.jpg)
One more leaving me and another struggling to breathe.
He didn't look good but still... You watch them suffer, and it's sad.
I'm still going, can't process it and don't want to.
17 April
Today, I'm still off work. I went to a protest and then to the hospital; I was waiting for a donation of masks. I give to the staff when I get donations. They were from N95FORNYC. They contacted me weeks ago and said they have stuff to give to medical workers. I said sure, whatever they want to give us...I'll take it and share it with the staff from different units and other hospitals.
-19-br.jpg)
I'm so angry. I saw the post about the monetary donations.[This is a fundraiser by celebrities such a Kim Kardashian and Ellen DeGeneres raising money for Mount Sinai hospital system in NYC] I'm upset because the hospital has been asking for money on our behalf and here, we are being asked to keep our N95 for the whole shift to recycle them.
No shoe covers, no head covers, half-open gowns. The food we get is from donations. The goggles I have were a donation. The shields are being saved on racks for reuse. So where is the money from the donations?
They have a page and commercials asking for donations for the healthcare workers. What are they doing with the money?

People are being told they only get seven days paid if they have to be out for COVID. Seven straight days not seven working days. For a nurse, that means three days only because we work long shifts and only three shifts a week and one week of the month we work 4. We only work 13 shifts a month.
I stay in my attic; I don't see my family. I can't get tested, and neither can my sick friends. I'm devastated and tired of fighting to get the same answer and to keep going around the same circle.
I'm back at work on Tuesday.
18 April
I went to bring food to my friend and coworker, who is quarantined in a hotel bedroom. She still hasn't gotten tested despite being symptomatic for over a week and her symptoms getting worse. She had a deadly cough, chest pain, body aches, fever, nausea, decreased appetite and they are still telling her from the hospital; they will see how she feels.

Why isn't she getting tested? Because the people in Employee Health Services are a bunch of incompetents. There is no good reason, and they change their testing criteria every day, and it is really up to the person on the phone than any real criteria.
Can you get a test privately? Me, no. Well, I have to go through hoops and hoops. I don't have symptoms so I would have to make an appointment and wait in a line or hours. You have to ask a doctor or have specific symptoms. You can't just go and say "I want to be tested", and it differs wherever you go. It's a mess; everyone says a different thing.
19 April
That's a bunny in one of the COVID units. They dressed it up with PPE, and I thought it was cute... It has a little note saying it was ready to do its part in fighting COVID. Not sure who did it, the manager, the secretary or the staff. Either way, it was done with the intention to keep spirits up.
-12-br.jpg)
The staff love donations. They are thankful, They have gotten so many things from people, restaurants, organisations.
Morale... There is no morale. We understand we have each other and the general public but everyone else abandoned us. We have us. For the most part, our managers are very supportive, but anyone else above them...It's a lost cause. We are on our own. Completely on our own.
20 April
I'm so upset!
Just found out my union, NYSNA, [New York State Nurses Association] who is supposed to fight for us and help us, not only has used and abused us collecting our dues but now has filed a lawsuit on behalf of one or two hospitals and left the rest of us out.
[On April 20, NYSNA sued the New York State Department of Health and two hospitals, Montefiore Medical Center and Westchester Medical Center, accusing them of failing to protect the health and safety of nurses treating COVID-19 patients.]
We all pay dues, and we are all struggling in the same way.
I have been fighting with them as some of their people failed to recognise our issues and allowed our situation to get worse.
And I have been personally attacked for raising my concerns. They said we were lying.
22 April
Today I'm on my Rehab unit converted to Non- COVID med-surg.
A patient who has been tested multiple times for COVID and tested negative...has all of the symptoms and I swabbed him again today...
This is the fifth time he gets tested. Same virus but a different strain....it appears to be mutating as it moves along.
Staffing levels? Today I started with three plus one admission. So four patients...but it's nonstop we are pretty busy.
After COVID, the hospitals were full...they said we could go up to 10 or 12 patients on the med-surg floors but they never really happened because so many people were dying. And also because they brought staff from other states and facilities owned by the hospital that closed.
As people start to come out and this thing continues to spread we don't really know what the future will bring...
I'm scared because we are all having a difficult time with the sacrifices for us and our families, and if people start to come up so soon and act reckless [if they stop self-isolating], I'm afraid we may end up where we started, with too many getting sick and not enough capacity or resources to help them.
I need to go back to my family, my kids need me...and this is more difficult emotionally than it is physically...
I'm young and healthy, and I can work long hours and days and be OK...but the pain of not being able to be around my husband and kids is taking a toll on me and on them.
March 19th was the last day I spend time with my kids.
My husband will bring me food sometimes and drop it off, and we see each other from a few feet away.
The kids know and understand, but they ask me not to come back here [the hospital] so that I can return home.

I worry for them...for their mental health and although they look OK...I don't know how OK they will be...do they feel abandoned? Do they think that I chose work over them?
But I have my boy 9 and my youngest girl 7 who really miss me more and need my hugs and kisses...can they really understand why I must be away from them?
I'm glad to be here...being alone and having time to think allows me to process and feel and I'd rather not.
It's too much, and I feel so helpless.
I cry and miss them...I would have never sacrificed my family and my children for any job, but the fear of exposing them and perhaps losing them has given me the strength and power to stay away.
23 April
My third shift of the week today.
My health? I'm good. I got my antibody test back, and I'm negative.
I don't have antibodies against it.
We had several patients with symptoms that already tested negative, but then you wonder, if they are still incubating, when will they turn positive?

I actually feel safer working with the confirmed COVIDs than with those who supposedly don't have it...and after several days of being symptomatic, finally, test positive.
When they are confirmed you just watch them closely and protect yourself as much as possible...having potentials or having to wonder who has or when will they get it...gives us anxiety and is more dangerous...
We have nurses who are pregnant, and I feel bad... I'm scared for them.
24 April
I was in charge and it was hectic.
I'm off today, resting as much as I can.
We're still getting admissions constantly.
Some COVID some non-COVID until proven otherwise.
Mostly people in pain.
Anything unusual yesterday? Besides the disorganization with all the changes from COVID and not knowing where we will get staff from and when.
We're still lacking supplies. Running crazy.
But we try our best and still show up to work despite the challenges.
-30-br.jpg)
Being in charge, that means you figure out the assignment, assist the other nurses, provide support basically and, depending on the situation, decision-making.
They would ask me for supplies. We had float nurses from other units. They would ask where certain things are or how they could get them.
Where to put the patients that were placed in isolation...in which rooms? Who could be moved to accommodate new admissions?
Throughout the day we needed different supplies and items we didn't have...I would ask for it or send the secretary.
I would assist them with doing something for their patients if they were busy or stuck doing something else.
I had my own patients but I had only 4...they all ended up with 5. And I had the same patients I had for 3 days so it was easier...I already knew the patients and could anticipate their needs better. They knew me and I knew them...it decreases anxiety...it saves you time if you can anticipate their needs and you know them.
I don't enjoy it...I don't mind helping as I always do...but being in charge gives you more responsibility and if you are busy it adds to the stress of having to figure something else out.
Ideally, a charge nurse is good assistance and support. If they don't have patients, you can really help out and make sure things run smooth...but that's not the case if you have your own assignment of patients.
I had a nurse who is pregnant...and one of her patients was showing symptoms of COVID. I felt so bad telling her that patient needed to be tested and although I performed the test for her, I felt really bad informing her.
I can't imagine her fear...my unit is supposed to be non-COVID but that does not mean they won't become COVID. We don't know what kind of exposure they have had and where...They didn't come to the hospital for COVID but some still end up positive because the virus incubates for very long.
It is not safe no matter what we do.
25 April
Today I did rest.
I went to pick up donations of facial products for healthcare workers suffering from skin irritation from the use of the N95 masks, and I went food shopping and to the pharmacy for my family.
I'll give the donations out on Monday when I go back.
My family are good...healthy. It's all that matters.
I listened to loud music in my car, while I drove an hour away to pick up the donations.
Enjoyed the nice day and fresh air...appreciating my deep breaths.

How do my patients feel about COVID? The patients that are aware and suspect they have COVID pending results, or haven't gotten tested, are afraid of having it...but once they get their diagnosis...most of them are unaware how they even got infected.
They are scared to death...they are afraid they will not make it...
I have had several young ones in their 30s, 40s ask me if I think they will make it...what do you tell them?
Yes you will...not knowing and seeing them struggle to breathe to the point where they can't really have a conversation without their oxygen dropping or even get up to walk to the bathroom.
Or tell them you don't know...adding to their fear
The only thing I could answer is that, right now, we keep our hope and faith that we will make it.
28 April
We are now starting to clean COVID units to convert them back to what they were pre-COVID...
There are barely any COVIDs in the ICU and they are starting to prepare for scheduled surgical procedures.
We can now breathe a little easier but still need to remain cautious and not let the guard down.
As we start to gain some normality, we can spend more time on checking on each other and working on healing from this experience.
It is the start a new and hopefully better beginning.
THE END